Mechanism of injury
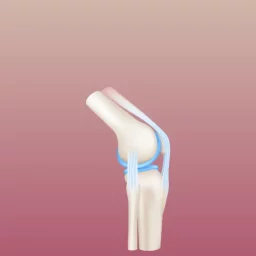
The knee is often referred to as the most complex joint in the human body and is subjected to large forces during sporting activities. These forces are resisted by a number of structures including the five main ‘static’ restraints of the knee: the two cruciate ligaments, the two collateral ligaments, and the popliteus tendon. The anterior cruciate ligament (ACL) is arguably the most important and well-known of these five structures; if the ACL was in the band N-Sync, for example, it would be Justin Timberlake!
Risk factors
Although a direct blow to the knee can injure the anterior cruciate ligament, you may be surprised to learn that almost 80% of injuries are caused by non-contact events involving a sudden deceleration or change in direction. In females, the rupture of the ACL is 2.5 times more likely than in males. The most cited reasons for these gender differences are:
- Reduced knee and hip bending during landing
- Increased “knock-kneed-ness” (greater genu valgum of the knee)
- Increased internal rotation of the thigh bone,
- High quadriceps activity unbalanced by the hamstrings
- The influence of the menstrual cycle
How do you know if you have torn your ACL?
The consistent description of ACL Injury includes twisting of the knee, feeling or hearing a pop, unable to continue the activity or even bear weight, or hemarthrosis as the knee fills up with blood very quickly because ACL has an abundant blood supply. As the pain settles, walking and running in a straight line is not usually a problem, but when attempting to turn or sidestep, the knee feels wobbly and the individual may demonstrate their instability by sliding their clenched fists against each other.
What do you do if you have torn your ACL?
After an ACL injury, deficits occur in strength, proprioception, muscle timing and gait patterns. In fact, strength and proprioception occur in an injured and non-injured limb. There are two approaches that can be taken post-ACL Injury – Operative and Conservative.
ACL reconstruction surgery is indicated in ACL-deficient patients with symptomatic instability or a desire to compete in high-risk activities.
Research has demonstrated that physiotherapy provided pre-operatively is effective in increasing strength and balance which may limit the number of episodes of ‘giving way’ and decrease the incidence of re-injury in the ACL deficient knee. However, surgery has a lot of associated risks and is considered an invasive type of treatment. Recent studies have shown that patients who underwent rehabilitation of the knee with a stable knee did not need surgery and had good outcomes with conservative care.
So if an ACL injury is confirmed, consider whether this is actually symptomatic (giving way) before rushing into surgery. ACL reconstructions aim to stabilize an unstable knee, but if it’s not unstable in the first place, conservative rehabilitation is best.
Return to play
After appropriate rehabilitation, a gradual return to sport is initiated at the six to nine-month mark. Only if the individual’s knee does not present with pain or effusion, during or after functional sport-specific training drills. The individual must also be able to demonstrate the appropriate strength and endurance needed for their specific sport.
How do I prevent an ACL Injury?
Anterior cruciate ligament injury rates appear to be on the increase. It is of concern that recent reports show the rates of ACL injury to have grown most rapidly at the younger end of the age spectrum.
Implementing an ACL injury prevention program can be extremely beneficial for all individuals. Keep in mind that this program will not prevent ACL tears from occurring but can help decrease the risk. There are five key steps that should be included in the planning of this program:
- Identification
- Exercises
- Training load and volume
- Training Frequency
- Exercise timing
As a helping hand, a physiotherapist is someone who commonly rehabs individuals following an ACL injury. They are capable of observing your movements, screening you for deficits, and helping you to correct them.
For more information or to book an appointment with one of our chiropractors, physiotherapists or massage therapists, visit our clinic websites at Curavita Byward and Curavita Glebe.
Byward Market
Email: info.byward@curavita.com
URL: https://byward.curavita.com
Glebe
Email: info.glebe@curavita.com
URL: https://glebe.curavita.com